Immuno-Oncology
Harnessing the body’s immune system to fight cancer

What is Immuno-Oncology?
Immuno-oncology, or immunotherapy, is a type of cancer treatment that uses the body’s own immune system to recognise and attack cancer cells.
The immune system consists of many different cells that form the body’s natural defence system against infection. These immune cells can also be used to fight cancer, but some tumours develop ways to hide from immune detection. Immunotherapy helps the immune system identify and attack cancer cells more effectively.
The most common immunotherapies are drugs called immune-checkpoint inhibitors, such as anti-PD-1. These drugs reactivate or “train” special immune cells called T cells that are located close to the cancer. Once activated, these T cells attack cancer cells throughout the body and can do so for long periods of time.
Other immunotherapies include specialised vaccines, T cell engagers (antibodies that link cancer cells with T cells together) and cell therapies.
In conditions such as melanoma, lung, kidney and certain breast cancers, immunotherapy has significantly improved long-term outcomes (> 5 years) for many patients.
Unlike traditional chemotherapy which causes side effects such as nausea, fatigue, infection and hair loss, immunotherapy can cause different side effects. Monitoring by doctors experienced in immuno-oncology is important to manage the potential side effects of immunotherapy quickly and safely.
Immune Checkpoint Inhibitors
Immune checkpoint inhibitors are a type of immunotherapy used to treat cancers such as melanoma, skin, lung cancer and kidney cancer. These medicines work by helping the body’s own immune system recognise and attack cancer cells.
The immune system uses natural “checkpoints” to prevent it from becoming overactive and damaging healthy tissues. One important checkpoint involves a protein called PD-1 (programmed cell death protein 1), which sits on immune cells known as T cells. Some cancer cells use this pathway to switch off the immune response and avoid being attacked.
Medicines known as anti-PD-1 therapies block this signal. By releasing this “brake”, T cells can recognise and target cancer cells more effectively. In melanoma and several other cancers, anti-PD-1 treatments have significantly improved long-term outcomes for many patients.
Because these treatments stimulate the immune system, they can sometimes cause inflammation in normal organs. This may affect the skin, bowel, thyroid, lungs or other parts of the body. Most side effects are manageable if identified early. Careful monitoring, regular review and prompt reporting of new symptoms are important to ensure treatment remains both safe and effective.
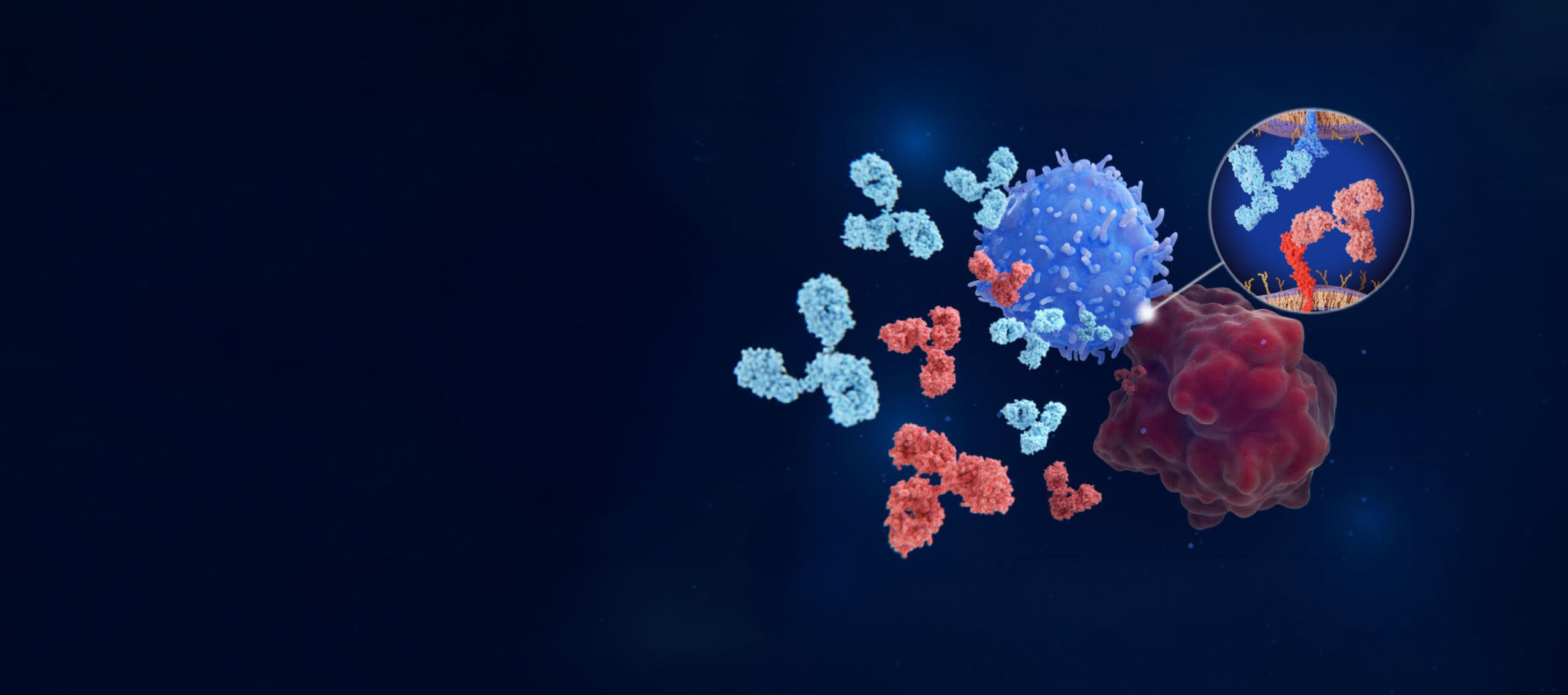
Description
Immune checkpoints regulate the immune system. Antibodies block the interaction between PD-L1 on cancer cells and PD-1 on T-cells, allowing T-cells to attack and kill cancer cells.
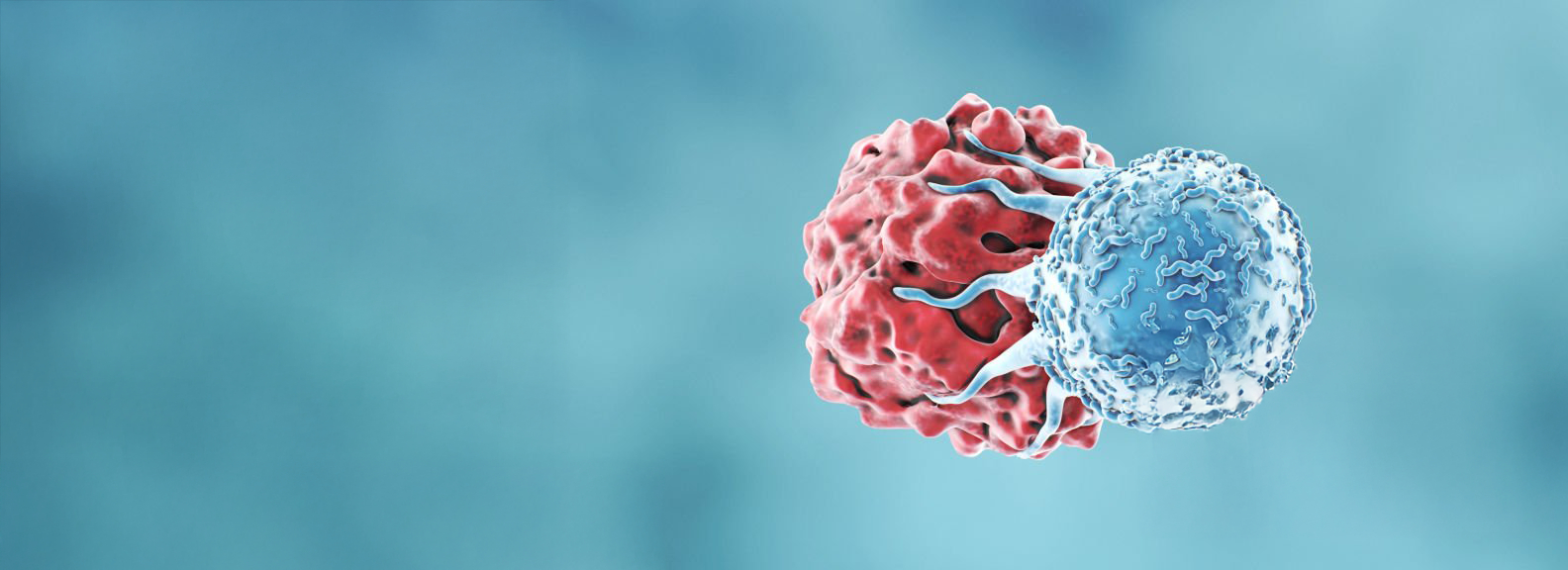
T cell (blue) attacking a cancer cell (red)
T Cell Engager
T cell engagers are a newer type of immunotherapy designed to help the immune system find and attack cancer cells more directly. They are laboratory-engineered antibodies that act like a bridge between cancer cells and immune cells called T cells.
Normally, T cells circulate through the body looking for abnormal cells. Some cancers can avoid detection or may not attract enough immune attention. T cell engagers work by attaching to a specific marker on the cancer cell and at the same time binding to a T cell. This brings the two cells into close contact, helping the immune system recognise and destroy the cancer cell more effectively. Examples of T cell engagers are tebentafusp which is licensed for use in patients with advanced uveal (ocular) melanoma.
Because these medicines activate immune cells, they can sometimes cause side effects related to immune activation, such as fever, rash or inflammation. Careful monitoring during treatment is important. T cell engagers are an evolving area of research and hold great promise for the treatment of cancer.
Cell Therapy
Cell therapy is a form of immunotherapy that uses a patient’s own immune cells to help fight cancer. Unlike standard medicines that are given directly into the bloodstream, cell therapy involves collecting immune cells, modifying or expanding them in a specialised laboratory, and then returning them to the patient to strengthen the immune response against cancer.
One example is tumour-infiltrating lymphocyte (TIL) therapy, where immune cells that have already entered the tumour are removed, multiplied in large numbers, and then infused back into the body. The goal is to enhance the body’s natural anti-cancer response. Other forms of cell therapy involve engineering immune cells to better recognise specific targets on cancer cells.
Cell therapy is a complex treatment that requires careful selection, preparation and monitoring.